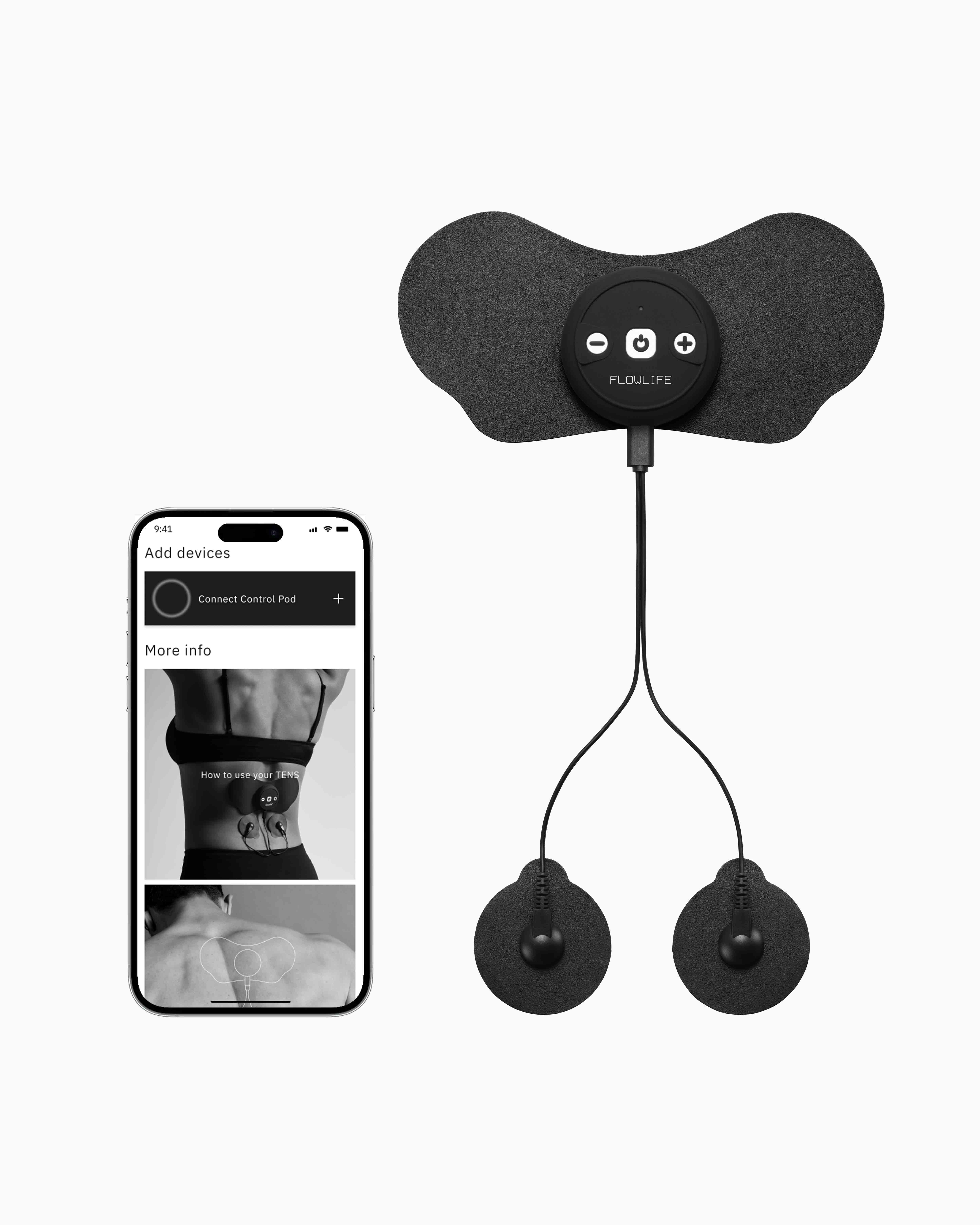
Flowtens Connect
150 EUR
)
Science
TENS therapy uses low-voltage electrical currents to interact directly with the nervous system, blocking pain signals and stimulating the body's own endorphin production. Unlike medication, it targets pain at the source without systemic side effects, making it one of the most clinically supported non-pharmacological tools for both acute and chronic pain management.
FAQ
How does TENS therapy work?
What conditions does TENS therapy help with?
What is the difference between TENS and EMS?
How should TENS electrodes be placed?
Is TENS therapy safe?
Can TENS therapy help with chronic pain?
How does TENS therapy differ from pain medication?
Can TENS therapy be used during exercise?
How often should TENS therapy be used?
Can TENS therapy help with nerve pain?
TENS therapy, which stands for transcutaneous electrical nerve stimulation, works by delivering low-voltage electrical pulses through the skin that interact with sensory nerve fibers, blocking pain signals from reaching the brain and stimulating the release of endorphins.
TENS works through two different mechanisms depending on the frequency used. At high frequency (80 to 150Hz), the electrical pulses activate large sensory nerve fibers that carry signals faster than those that carry pain signals. These fast-moving signals essentially race the pain signals to the spinal cord and block them at the gate, a well-established mechanism called gate control theory. The result is immediate pain relief during and shortly after the session. At low frequency (2 to 10Hz), electrical pulses activate deeper nerve fibers, triggering the body to release its own natural painkillers, endorphins and enkephalins, producing longer-lasting pain relief that continues after the session ends.
TENS is one of the most extensively researched non-pharmacological pain management tools available. Studies consistently show significant reductions in acute and chronic pain across musculoskeletal, neuropathic, and post-surgical conditions. Multiple systematic reviews confirm the effectiveness of TENS for pain relief with a strong safety profile.
High-frequency TENS produces immediate pain relief that lasts during and shortly after the session. Low-frequency TENS produces slower-onset relief that persists for hours after use. Most devices allow adjustment of frequency and intensity to match the type and location of pain.
Explore
)
TENS therapy is effective across a wide range of pain conditions, including musculoskeletal pain, neuropathic pain, post-surgical pain, and chronic pain syndromes, making it one of the most versatile pain management tools available without a prescription.
Placing TENS electrodes near the source of pain activates sensory nerves in that specific area. For musculoskeletal pain, including lower back, neck, and joint pain, high-frequency TENS provides rapid local relief via the gate-control mechanism. For neuropathic pain, caused by nerve damage or dysfunction, low-frequency TENS activates endorphin pathways, providing more systemic and longer-lasting analgesia. Post-surgical pain responds to both frequencies depending on the type and location. TENS is also used effectively for dysmenorrhoea (period pain), fibromyalgia, CRPS, and cancer-related pain.
Systematic reviews and meta-analyses confirm significant pain reductions with TENS for chronic lower back pain, osteoarthritis, fibromyalgia, and neuropathic pain. Research confirms pain reductions comparable to those of mild analgesics, with a significantly better side-effect profile.
Experiment with electrode placement to find the most effective positions for your specific pain. Place electrodes around or on either side of the pain area rather than directly on top of it. Start with high-frequency for immediate relief and test low-frequency for more sustained effects.
Explore
)
TENS and EMS are both electrical stimulation modalities, but with distinct goals. TENS targets sensory nerve fibers to relieve pain. EMS targets motor nerve fibers to produce muscle contractions.
TENS delivers electrical signals at frequencies and intensities that prioritize sensory nerve activation, engage the gate control mechanism, and activate endorphin pathways for pain relief, without producing noticeable muscle contractions. EMS delivers electrical signals at frequencies and intensities that activate motor nerves and produce actual muscle contractions, used for muscle rehabilitation, strength training, and preventing muscle atrophy. Combination TENS/EMS devices allow users to adjust parameters to achieve pain relief, muscle activation, or both, depending on the therapeutic goal.
Research confirms clear differences in nerve targeting and physiological effects between TENS and EMS. Studies show TENS is superior for pain relief, while EMS is more effective for muscle activation and rehabilitation.
Choose TENS mode for pain relief and recovery. Choose EMS mode for muscle activation, rehabilitation, and strength maintenance. Many modern devices combine both, providing flexibility for different therapeutic needs.
Explore
)
Electrode placement determines the effectiveness of TENS therapy. Electrodes should be placed on either side of, around, or proximal to the pain area, not directly over bony prominences, joints, or sensitive skin.
TENS works by activating sensory nerve fibers in the treated area. Optimal placement maximizes the density of nerve fibers within the electrical field. For muscle pain, place electrodes around the pain area to create an electrical field through the affected musculature. For neuropathic pain, place electrodes proximal to the pain distribution along the nerve pathway. Avoid placing them directly over bones, joints, the spine, wounds, irritated skin, implanted metal devices, or areas near a pacemaker.
Clinical guidelines for TENS electrode placement are well-established and consistently validated in research and clinical practice. Studies confirm that optimized electrode placement produces significantly stronger pain relief than suboptimal positioning.
Experiment systematically with electrode placement to find the configuration that produces the best relief for your specific pain pattern. Refer to your device's manual for recommended placement configurations for common pain conditions.
Explore
)
TENS therapy is safe for most individuals when used according to device guidelines. It is contraindicated in people with implantable electronic medical devices, including pacemakers and implantable cardioverter-defibrillators.
TENS devices deliver very low-voltage electrical currents that do not cause tissue damage at recommended intensity levels. The electromagnetic field from TENS can interfere with implanted electronic devices, which is why pacemaker and ICD patients cannot use it. Epilepsy is a relative contraindication. Electrode placement should avoid the neck (carotid nerve region), directly over the heart, the temple area, damaged skin, and during pregnancy without medical guidance.
TENS has an exceptional safety profile, supported by decades of clinical research and use. Adverse events are rare and limited to mild skin irritation at electrode sites, which typically resolves with adjustment of the gel or electrode position.
Always start at the lowest intensity setting and increase gradually until you feel a comfortable tingling sensation. Avoid intensities that produce pain or discomfort. Consult a physician if there is a history of epilepsy, heart conditions, or implanted devices.
Explore
)
TENS therapy is one of the most well-documented non-pharmacological tools for chronic pain management, with clinical evidence supporting its effectiveness across a wide range of chronic pain conditions.
Chronic pain often involves central sensitization, a state where the pain-processing nervous system becomes hypersensitive and generates pain signals even when there is no ongoing tissue damage. Low-frequency TENS tells the body to release its own natural painkillers, endorphins, which work through the same receptors as pain medication but without the side effects or dependency risk. With regular use, this can gradually calm down a pain system that has become oversensitive, raising the threshold at which pain is felt. High-frequency TENS provides symptomatic relief through the gate mechanism, which is effective for flares and worsening episodic pain.
Systematic reviews confirm significant pain reductions with TENS for chronic lower back pain, fibromyalgia, neuropathic pain, and arthritis-related pain. Research shows that regular TENS use reduces dependence on pain medication and improves functional status in chronic pain patients.
For chronic pain, use TENS consistently, daily or multiple times per week, rather than only during flares. Combining high- and low-frequency TENS in the same session addresses both immediate symptoms and the underlying central sensitization mechanisms.
Explore
)
TENS provides pain relief without systemic side effects, dependency risk, or drug interactions. It works through nervous system modulation and the body's own endogenous opioid pathways rather than through systemic pharmacology.
Analgesics like paracetamol and NSAIDs work throughout the body and produce side effects, gastrointestinal problems, kidney toxicity, and cardiovascular risk with chronic use. Opioid analgesics carry dependency potential, tolerance development, and cognitive side effects. TENS targets pain neurologically at its source, activates endogenous opioid pathways without dependency risk, and uses the gate mechanism without system-wide neurochemical changes. There are no drug interactions, no contraindications based on organ function, and no tolerance development with appropriate parameter variation.
Research confirms that TENS produces pain relief comparable to that of mild analgesics for musculoskeletal and neuropathic pain, with a significantly better side-effect profile. Studies show reduced analgesic use in patients who integrate TENS into their pain management protocols.
TENS and medication serve complementary roles. Medication is appropriate for acute pain flares where fast systemic relief is needed. TENS is most appropriate as a daily management tool for chronic pain, as a complement to or a reduction in pharmacological treatment.
Explore
)
TENS therapy is generally not suitable during active physical training, but can be used effectively during rehabilitation exercises with a limited range of movement.
TENS electrodes require stable skin contact and connected wiring, which limit freedom of movement during full training. During rehabilitation exercises, light strength training, or functional movement work with limited electrical interference, TENS can be applied to provide pain relief during movement and improve movement quality. TENS during rehabilitation exercises often improves range of motion and exercise quality by reducing the protective muscle tension and pain-inhibited movement that limits rehabilitation progress.
Clinical research supports the use of TENS during rehabilitation exercises to improve functional movement recovery. Studies show that TENS during movement-based rehabilitation produces faster functional outcomes compared to TENS or training alone.
Use TENS during light rehabilitation exercises and mobility work to relieve pain and improve movement quality. Avoid during high-intensity or cardiovascular training. Consult your device manual for activity-specific guidelines.
Explore
)
TENS therapy can be used daily and multiple times per day for pain management without risk of dependency or tolerance development with appropriate parameter variation.
Unlike opioid medication, TENS does not produce receptor downregulation or dependency with regular use. However, the gate-control pain relief effect can become less pronounced if the same parameters are used repeatedly at the same location, the nerve receptors adapt to the stimulus. Periodically varying electrode placement, frequency, and intensity resets the response. Daily use for chronic pain is safe and supported by clinical guidelines. Regular low-frequency use produces cumulative endorphin effects that may gradually reduce baseline pain sensitivity.
Clinical guidelines for chronic pain management consistently recommend TENS as a daily or multiple-times-daily intervention. Studies confirm safe daily use without adverse effects from regular application.
For chronic pain, use TENS for 20 to 60 minutes per session, one to three times daily, at the affected area. For post-exercise recovery, a single 20 to 30-minute session immediately after training. Vary electrode placement and parameters regularly to maintain effectiveness.
Explore
)
TENS therapy reduces neuropathic pain by modulating the abnormal nerve signaling that drives it, using both the gate control mechanism and endorphin pathways to interrupt the pain cycle.
Neuropathic pain occurs when sensory nerve fibers are damaged, compressed, or sensitized, producing spontaneous pain, allodynia (pain from non-painful stimuli), and hyperalgesia (amplified pain responses). High-frequency TENS activates fast A-beta nerve fibers, which inhibit the slower pain-carrying fibers via the gate mechanism, reducing abnormal pain signaling. Low-frequency TENS triggers the release of the body's own natural painkillers, which act on the spinal cord and brain to reduce the oversensitivity that is often behind nerve pain.
Research supports TENS as an effective intervention for multiple neuropathic pain conditions, including diabetic neuropathy, post-herpetic neuralgia, and carpal tunnel syndrome. Studies confirm measurable reductions in neuropathic pain intensity and improved quality of life with regular TENS use.
For nerve pain, electrode placement along the nerve pathway proximal to the pain site is often more effective than placement directly on the pain area. Low-frequency TENS at 2 to 10Hz produces more lasting effects for neuropathic pain than high-frequency protocols.
Explore
)
FAQ
Explore